Move Better, Feel Better, Live Better!
Get expert physical therapy services and a personalized plan that’s right for you to feel better quickly.
Don’t Let Pain or Injury Hold You Back
Delaying proper treatment of your symptoms can lead to:
Get the Care You Deserve
Personalized Physical Therapy For Exceptional Results
The Main Focus is Always on You
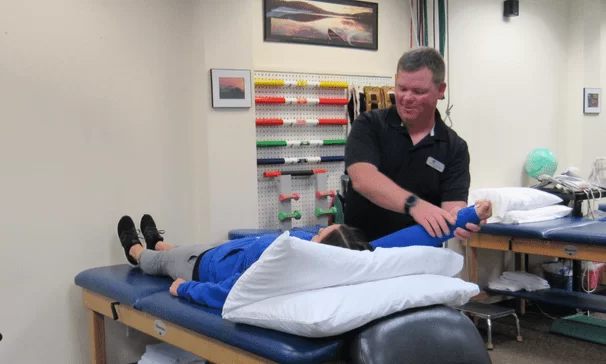
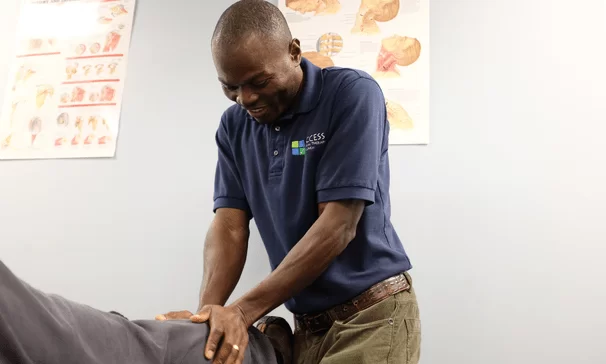
The moment you walk through our doors you’ll experience kindness, respect, and a team dedicated to creating a positive space where you feel heard, valued, and understood.
Your Own Customized Care Plan
That’s why we believe in the power of personalized treatment plans based on a thorough one-on-one evaluation, designed to help you achieve fast, lasting results.
Quick relief from pain and discomfort
Our team of professionals uses the latest techniques and technologies to deliver fast, effective treatment, so you can get back to living the life you love as soon as possible.
Convenient Locations
Satisfied Patients
Expert Therapists
Your Partner in Fast, Effective Pain Relief
At ACCESS PT, we understand the frustration and disappointment of living with pain and injury. That’s why we focus on fast, effective treatment to help you get back to your active lifestyle as quickly as possible. Our highly educated team of therapists are dedicated to helping you move better, feel better, and live better, while building lasting connections that create exceptional outcomes.
If you’re ready to live pain-free and get better quickly, Request an Appointment or Call Us today to schedule your first appointment.
Discover Our Success Stories
Discover Our Story
Listen to our founders, Chris and Steve Albanese, as they share their inspiring journey and the motivation behind establishing Access PT & Wellness. Learn about their passion for helping people and their commitment to offering exceptional services to all patients.
Personalized Care for a Variety of Conditions
We offer comprehensive care for a range of common conditions and issues, including:

Start Your Journey to a Pain-Free Life
01
Schedule your first appointment
Contact us to schedule your initial evaluation, where we’ll get to know you and your unique needs. During this one-on-one evaluation, your therapist will conduct a comprehensive physical assessment and discuss your medical history, lifestyle, and goals for treatment.
02
Get a personalized care plan
We’ll create a personalized care plan that fits your lifestyle and goals. Your therapist will use their expertise to develop a customized treatment plan that addresses your unique needs, using a variety of techniques and modalities to help you achieve your goals.
03
Achieve fast, lasting results
Our dedicated therapists utilize the latest techniques and technologies to provide you with the fast, effective treatment you need to achieve lasting results. We are committed to working with you to help you move better, feel better, live better.
Personalized Physical Therapy for Lasting Wellness
At ACCESS PT, we understand that no two patients are alike. That’s why our approach is centered around you, your needs, and your goals. We believe that the key to exceptional outcomes is personalized care that is tailored to your unique circumstances. Our team of experts is dedicated to creating a supportive, positive environment that fosters growth and learning, so you can achieve your goals and live a pain-free life.
What sets us apart is our commitment to patient-centered care. We take the time to get to know you, your lifestyle, and your specific needs so we can design a customized treatment plan that is attuned to your goals. Our expert therapists utilize the latest techniques and technologies to provide you with the fast, effective treatment you need to achieve lasting results.
We are dedicated to working with you every step of the way to help you achieve exceptional outcomes and live a pain-free life.
Whether you’re recovering from an injury, managing a chronic condition, or looking to enhance your performance, we’re here to help you move better, feel better, and live better.
Don’t let pain or discomfort hold you back from living your best life.
Contact us today to schedule your first appointment and take the first step towards a healthier, happier you.

Learn About Your Insurance Options
We accept most major private insurance companies, Medicare and Medicare Supplements, Workman’s Compensation, and auto insurance claims.
We’re committed to helping you understand your insurance coverage and ensuring that your benefits are maximized, so you can get the care you need without breaking the bank.
Frequently Asked Questions
Reach out if you can’t find what you’re looking for.
New York
Connecticut
Pennsylvania
North Carolina